Expo
view channel
view channel
view channel
view channel
view channel
view channel
Medical Imaging
AI
Surgical TechniquesPatient CareHealth ITPoint of CareBusiness
Events
Webinars

- Collaboration Brings Continuous Monitoring to Metabolic Care Management
- FDA-Cleared Transseptal Access Device Enables Site-Specific Left Atrial Puncture
- Low-Frequency Wireless Sensor Monitors Arterial Stiffening and Blood Pressure
- AI Tool Estimates CPAP Effect on Cardiovascular Risk in Sleep Apnea
- Wearable AI Tool Predicts Hospitalization Risk in Heart Failure
- New Powered Stapler Enhances Intraoperative Feedback and Articulation
- New Pacing Approach Cuts Complications in Heart Failure Patients
- New Navigation-Guided System Enhances Precision in SI Joint Fusion
- Spine Surgical Table and Smart Stretcher Streamline Positioning and Transfers
- MRI-Guided Ultrasound Ablation Shows Faster Recovery Than Prostatectomy
- Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
- VR Training Tool Combats Contamination of Portable Medical Equipment
- Portable Biosensor Platform to Reduce Hospital-Acquired Infections
- First-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
- GE HealthCare and Medtronic Expand Alliance with Intraoperative Imaging Integration
- External Liver Assist System Receives FDA RMAT Designation
- New Partnership Expands Access to Predictive Tool for Patient Monitoring
- GE HealthCare Leads Major European Initiative to Advance Cardio-Oncology Care
- Medtronic and GE HealthCare Broaden Alliance Across Monitoring and Care Solutions
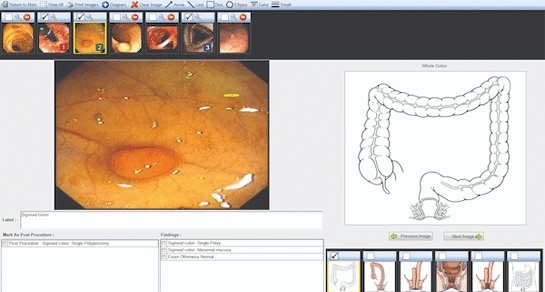
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
- Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
- Smartwatches Could Detect Congestive Heart Failure
- Versatile Smart Patch Combines Health Monitoring and Drug Delivery
- Algorithm Identifies Cardiac Arrest Hotspots to Guide AED Placement
- AI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
- Machine Learning Approach Enhances Liver Cancer Risk Stratification
- New AI Approach Monitors Brain Health Using Passive Wearable Data
- AI Tool Maps Early Risk Patterns in Bloodstream Infections

 Expo
Expo
- Collaboration Brings Continuous Monitoring to Metabolic Care Management
- FDA-Cleared Transseptal Access Device Enables Site-Specific Left Atrial Puncture
- Low-Frequency Wireless Sensor Monitors Arterial Stiffening and Blood Pressure
- AI Tool Estimates CPAP Effect on Cardiovascular Risk in Sleep Apnea
- Wearable AI Tool Predicts Hospitalization Risk in Heart Failure
- New Powered Stapler Enhances Intraoperative Feedback and Articulation
- New Pacing Approach Cuts Complications in Heart Failure Patients
- New Navigation-Guided System Enhances Precision in SI Joint Fusion
- Spine Surgical Table and Smart Stretcher Streamline Positioning and Transfers
- MRI-Guided Ultrasound Ablation Shows Faster Recovery Than Prostatectomy
- Revolutionary Automatic IV-Line Flushing Device to Enhance Infusion Care
- VR Training Tool Combats Contamination of Portable Medical Equipment
- Portable Biosensor Platform to Reduce Hospital-Acquired Infections
- First-Of-Its-Kind Portable Germicidal Light Technology Disinfects High-Touch Clinical Surfaces in Seconds
- Surgical Capacity Optimization Solution Helps Hospitals Boost OR Utilization
- GE HealthCare and Medtronic Expand Alliance with Intraoperative Imaging Integration
- External Liver Assist System Receives FDA RMAT Designation
- New Partnership Expands Access to Predictive Tool for Patient Monitoring
- GE HealthCare Leads Major European Initiative to Advance Cardio-Oncology Care
- Medtronic and GE HealthCare Broaden Alliance Across Monitoring and Care Solutions
- Voice-Driven AI System Enables Structured GI Procedure Documentation
- EMR-Based Tool Predicts Graft Failure After Kidney Transplant
- Printable Molecule-Selective Nanoparticles Enable Mass Production of Wearable Biosensors
- Smartwatches Could Detect Congestive Heart Failure
- Versatile Smart Patch Combines Health Monitoring and Drug Delivery
- Algorithm Identifies Cardiac Arrest Hotspots to Guide AED Placement
- AI Analysis of Pericardial Fat Refines Long-Term Heart Disease Risk
- Machine Learning Approach Enhances Liver Cancer Risk Stratification
- New AI Approach Monitors Brain Health Using Passive Wearable Data
- AI Tool Maps Early Risk Patterns in Bloodstream Infections